最適化されたソリューション、専門的なバルブの知識、業界ニュースを共有する
ご希望の用語やキーワードを入力すると、検索結果に関連記事が表示されます。お探しの回答が見つからない場合は、お気軽にお問い合わせください。喜んでお手伝いいたします。または、beauty@shefmon.comまで直接メールでお問い合わせください。
尿失禁の改善:膀胱コントロールと骨盤の健康を向上させるための最新ソリューション
- 管理者
尿失禁の改善
Urinary incontinence is one of those health concerns that people rarely talk about openly, yet it affects millions of women and men around the world. The truth is, losing bladder control is not just a physical issue—it can quietly impact confidence, social life, and emotional well-being. The good news? Modern pelvic health technologies are changing everything. From pelvic floor stimulation chairs to advanced laser therapies, improving urinary incontinence is more achievable today than ever before.
Let’s explore how urinary incontinence happens, what causes it, and—most importantly—how new technology like EMS chairs and fractional CO2 lasers can help restore control and confidence.
尿失禁について理解する
Urinary incontinence refers to the involuntary leakage of urine. It can range from occasional small leaks when sneezing to a complete loss of bladder control. While it may sound simple, the condition is actually complex and often linked to weakened pelvic muscles, nerve issues, or hormonal changes.
Recent clinical research highlights that pelvic floor dysfunction is one of the most significant contributors to bladder control problems. Strengthening and retraining these muscles plays a key role in recovery and long-term improvement.
尿失禁とは何ですか?
In simple terms, urinary incontinence is when the bladder cannot hold urine properly. This may happen because the muscles responsible for control are weak or overactive. It can occur temporarily or become chronic depending on the underlying cause.
Many patients experience embarrassment or delay treatment, but medical professionals emphasize early intervention for better outcomes.
Main Types of Urinary Incontinence
There are different forms of urinary incontinence, and understanding them helps choose the right treatment approach.
腹圧性尿失禁
This occurs when physical pressure—like coughing, sneezing, laughing, or lifting—causes urine leakage. It is especially common in postpartum women due to weakened pelvic muscles.
切迫性尿失禁
This type involves a sudden, intense urge to urinate followed by involuntary leakage. It is often linked to an overactive bladder.
Causes and Risk Factors
Urinary incontinence does not happen randomly. It is usually connected to specific physical changes or health conditions.
Pregnancy and Postpartum Changes
Pregnancy stretches pelvic muscles significantly. After childbirth, these muscles may remain weakened, leading to leakage issues. This is one of the most common causes in women.
老化とホルモンの変化
As people age, muscle strength naturally declines. Hormonal changes—especially during menopause—can also reduce bladder and urethral support, increasing risk.
骨盤底の健康が重要な理由
The pelvic floor is often described as the “hidden foundation” of bladder control. When it weakens, everything above it becomes unstable.
Role of Pelvic Floor Muscles
These muscles act like a supportive hammock for the bladder, uterus, and bowel. When strong, they help maintain continence effortlessly.
Muscle Weakness and Bladder Leakage
Weak pelvic muscles struggle to maintain pressure against the bladder, especially during movement or strain. This leads to leaks that can become more frequent over time.
Traditional Treatment Methods
Before modern technologies, most treatments focused on exercise and behavioral changes.
Pelvic Floor Muscle Training (PFMT)
PFMT, commonly known as Kegel exercises, is still considered a first-line treatment. Studies show it can significantly improve mild to moderate incontinence when performed consistently over time.
Lifestyle and Behavioral Changes
Doctors often recommend reducing caffeine intake, maintaining a healthy weight, and scheduling bathroom visits to train the bladder.
However, not everyone achieves full improvement with these methods alone.
Modern Technology for Urinary Incontinence Improvement
Today’s medical aesthetics and rehabilitation technologies offer non-invasive solutions that go beyond traditional exercises.
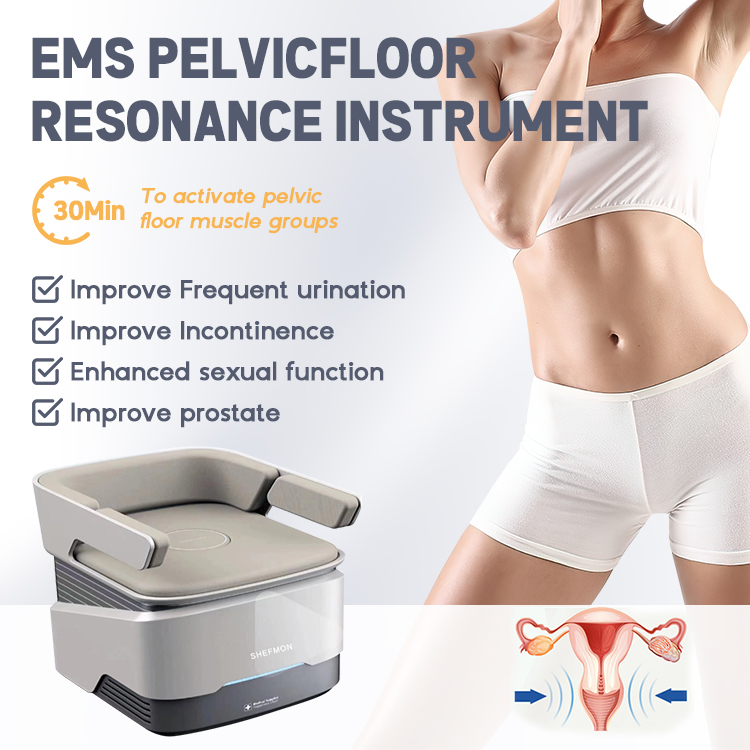
EMS Chair Therapy and Electromagnetic Stimulation
One of the most promising innovations is electromagnetic muscle stimulation (EMS) chairs. These devices use high-intensity focused electromagnetic energy to stimulate thousands of pelvic floor contractions in a single session.
A systematic clinical review found that magnetic chair therapies significantly improved urinary incontinence scores and pelvic muscle strength, with some studies reporting up to 70% symptom reduction in certain patients .
Interestingly, research also shows improved sexual function and quality of life alongside bladder control improvements, making it a holistic therapy for pelvic health .
Clinical Insights and Effectiveness
Recent studies comparing electromagnetic stimulation with traditional pelvic exercises show encouraging results. In many cases, combining therapies leads to better outcomes than exercise alone.
This is where professional-grade devices like those from SHEFMON come into play.
SHEFMON Advanced Treatment Solutions
SHEFMON specializes in professional beauty and rehabilitation equipment designed for clinics and medical spas. Their technologies focus on pelvic floor recovery, tissue regeneration, and non-invasive body improvement.
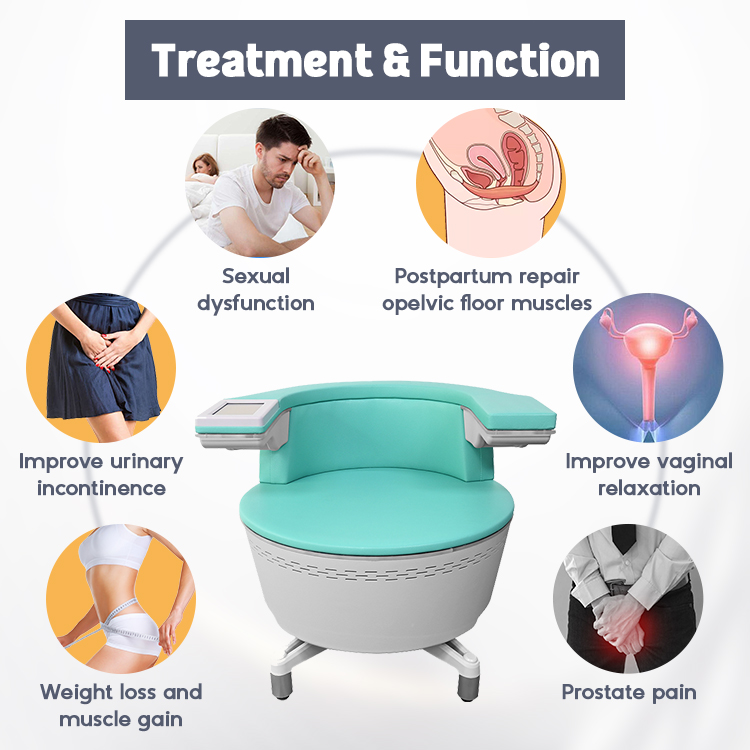
EMS Pelvic Floor Chairs for Recovery
SHEFMON offers advanced EMS chair systems designed for postpartum recovery and urinary incontinence improvement.
- E0435 Women’s Postpartum Repair EMS Chair
- E0436 電磁骨盤底筋リハビリテーション EMSチェア
These chairs stimulate deep pelvic contractions that cannot be achieved through voluntary exercise alone. Patients simply sit on the device while it activates muscle training cycles automatically.
The result? Improved bladder control, stronger pelvic muscles, and enhanced core stability over time.
CO2 Fractional Laser for Tissue Rejuvenation
Beyond muscle stimulation, tissue health is equally important. Fractional CO2 lasers help regenerate and tighten soft tissues, supporting long-term pelvic health.
2910nm Fiber Fractional CO2 Laser
SHEFMON 2910nm ファイバーフラクショナル CO2 ウルトラレーザー
This system focuses on controlled tissue stimulation, encouraging collagen regeneration and improved elasticity.
10600nm CO2 Scar Removal Laser
A0529 CO2フラクショナルレーザー装置
This device is commonly used for skin resurfacing and scar reduction, but it also supports tissue repair and rejuvenation in surrounding pelvic areas.
Research on CO2 laser therapy combined with pelvic exercises shows measurable improvements in urinary incontinence symptoms and quality-of-life scores .
Combining Therapies for Better Results
The future of urinary incontinence treatment is not about choosing one solution—it is about combining methods strategically.
Synergy of EMS and Laser Treatments
When EMS pelvic stimulation is combined with CO2 laser therapy, patients benefit from both muscle strengthening and tissue regeneration.
- EMS strengthens the pelvic floor muscles
- CO2 laser improves tissue elasticity and healing
- Together, they enhance bladder control stability
Clinical evidence suggests that multi-therapy approaches often outperform single-method treatments in long-term outcomes.
Benefits of Improved Urinary Incontinence Management
When urinary incontinence improves, the change goes far beyond physical symptoms.
Physical and Emotional Improvements
Patients often experience:
- より良い排尿コントロール
- Increased confidence in daily activities
- Reduced anxiety about leakage
- Improved sexual health and comfort
- Enhanced overall quality of life
In many cases, patients describe it as “getting their life back,” especially after postpartum or age-related changes.
結論
Improving urinary incontinence is no longer limited to exercises and lifestyle adjustments. With modern EMS議長 therapy and fractional CO2レーザー technology, pelvic floor rehabilitation has entered a new era. These treatments provide non-invasive, effective, and clinically supported solutions for restoring bladder control and confidence.
SHEFMON’s advanced medical aesthetic devices combine innovation with practicality, offering clinics and practitioners powerful tools to help patients achieve real results. Whether used alone or in combination, these technologies represent a major step forward in pelvic health care.
よくある質問
1. What is the fastest way to improve urinary incontinence?
The fastest improvements often come from combining pelvic floor exercises with EMS chair therapy, which stimulates deep muscle contractions.
2. Are EMS chairs safe for urinary incontinence treatment?
Yes, clinical studies show EMS pelvic stimulation is non-invasive and generally well tolerated with minimal side effects.
3. How long does it take to see results from EMS treatment?
Many users report improvements after 3–6 sessions, although full results depend on individual conditions.
4. Can CO2 laser help urinary incontinence?
CO2 laser therapy may improve tissue elasticity and support pelvic health, especially when combined with muscle training.
5. Is urinary incontinence permanent?
Not always. Many cases improve significantly or are fully managed with proper treatment, exercise, and technology-assisted therapy.